Compliance Confidence
How to Respond to a Marketplace Appeal Notice
How to Respond to a Marketplace Appeal Notice
Each year, after the Healthcare Marketplace’s open enrollment period ends, employers often begin to receive Marketplace Appeal Notices.
The letter notifies employers of employees who enrolled in Marketplace coverage and obtained an advanced premium tax credit for at least one month of the calendar year. Each letter identifies the employer, reason for the appeal notice, the employee, as well as the appeals process and timing.
What should employers do?
- Determine Internal Procedures for Responding
- Train Employees
- Pull Employee Records
- If Employee Was Offered Coverage, Appeal
The employer must respond within 90 days of the letter. The appeal does not impose or exempt the employer from employer shared responsibility penalty.
Designate and train an individual in the company to respond to the appeal notice and know when a qualifying offer was/was not made.
Employment records such as the employees full-time, part-time, or independent contract status, as well as benefits eligibility, offer, and waiver information will be particularly helpful in responding to the notice.
Complete the appeal form with any applicable attachments. Discuss with the employee the nature of the appeal and keep records of your response.
What Other Information Might an Employer Need?
Company Name
Company Address
Employer ID Number
Primary Contact Name
Primary Contact Address
Primary Contact Phone
Primary Contact Title
Secondary Contact
Employee Name
Employee Date of Birth
Marketplace Notice Date
Employee Application ID
Employment Status
Date of Offer of Coverage
Coverage MV and MEC
Affordability Safe Harbor
EE Cost of Coverage
Date Enrolled or Waived
Supporting Documents
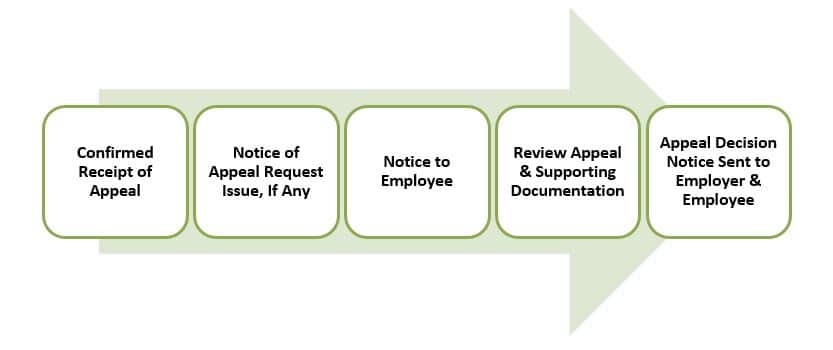
What Happens After Filing an Appeal?
OneDigital’s team of compliance experts have your back when it comes to meeting compliance requirements and steering clear of any penalties. Reach out to your OneDigital consultant to discuss your organization’s current situation.





